Search
Graham Jane Shannon Hall Pillow Simpson BAppSci PhD CRFS FANZSRS FThorSoc FERS BMedSci (Dist) MBBS, PhD (Dist) FRACP BMedSci (hons), PhD Honorary
The importance of lung recruitment before surfactant administration has been shown in animal studies. Well designed trials in preterm infants are absent. We aimed to examine whether the application of a recruitment manoeuvre just before surfactant administration, followed by rapid extubation (intubate-recruit-surfactant-extubate [IN-REC-SUR-E]), decreased the need for mechanical ventilation during the first 72 h of life compared with no recruitment manoeuvre (ie, intubate-surfactant-extubate [IN-SUR-E]).
Jane Pillow BMedSci (Dist) MBBS, PhD (Dist) FRACP Head, Developmental Chronobiology jane.pillow@thekids.org.au Head, Developmental Chronobiology
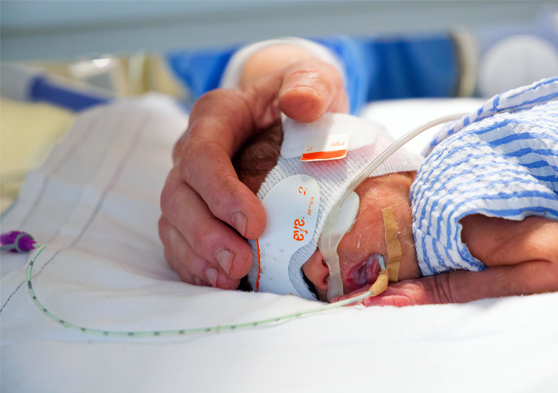
The CIRCA DIEM Study is a clinical research study being coordinated by the Chronobiology Team at The Kids Research Institute Australia, who are based in Perth, Western Australia and involving research teams from around the world.

The CIRCA DIEM study is a multicentre, prospective, open, blinded end-point (PROBE) parallel controlled study which aims to compare long term neuro-developmental outcomes of premature babies cared for in a cycled environment to premature babies who receive routine care in a non-cycled environment.

The CIRCA DIEM Study is a multicentre study, involving several different hospital sites across Australia. Here, you can find out more about which hospitals recruit babies into the CIRCA DIEM Study.

The CIRCA DIEM Study is a clinical research study being coordinated by the Chronobiology Team at Telethon Kids Institute, who are based in Perth, Western Australia and involving research teams from around the world.
Since the first description of bronchopulmonary dysplasia (BPD), multiple definitions to diagnose BPD and its grading have been published. Several studies have compared the predictive performance of these definitions for long-term outcomes. The objective was to identify the BPD definition with the optimal predictive performance for long-term respiratory and neurological outcomes in preterm infants.
Surfactant is a well-established therapy for preterm neonates affected by respiratory distress syndrome (RDS). The goals of different methods of surfactant administration are to reduce the duration of mechanical ventilation and the severity of bronchopulmonary dysplasia (BPD); however, the optimal administration method remains unknown.
Data on static compliance of the chest wall (Ccw) in preterm infants are scarce. We characterized the static compliance of the lung and Ccw to determine their relative contribution to static compliance of the respiratory system in very preterm infants at 36 wk postmenstrual age. We also aimed to investigate how these compliances were influenced by the presence of bronchopulmonary dysplasia and impacted breathing variables.
